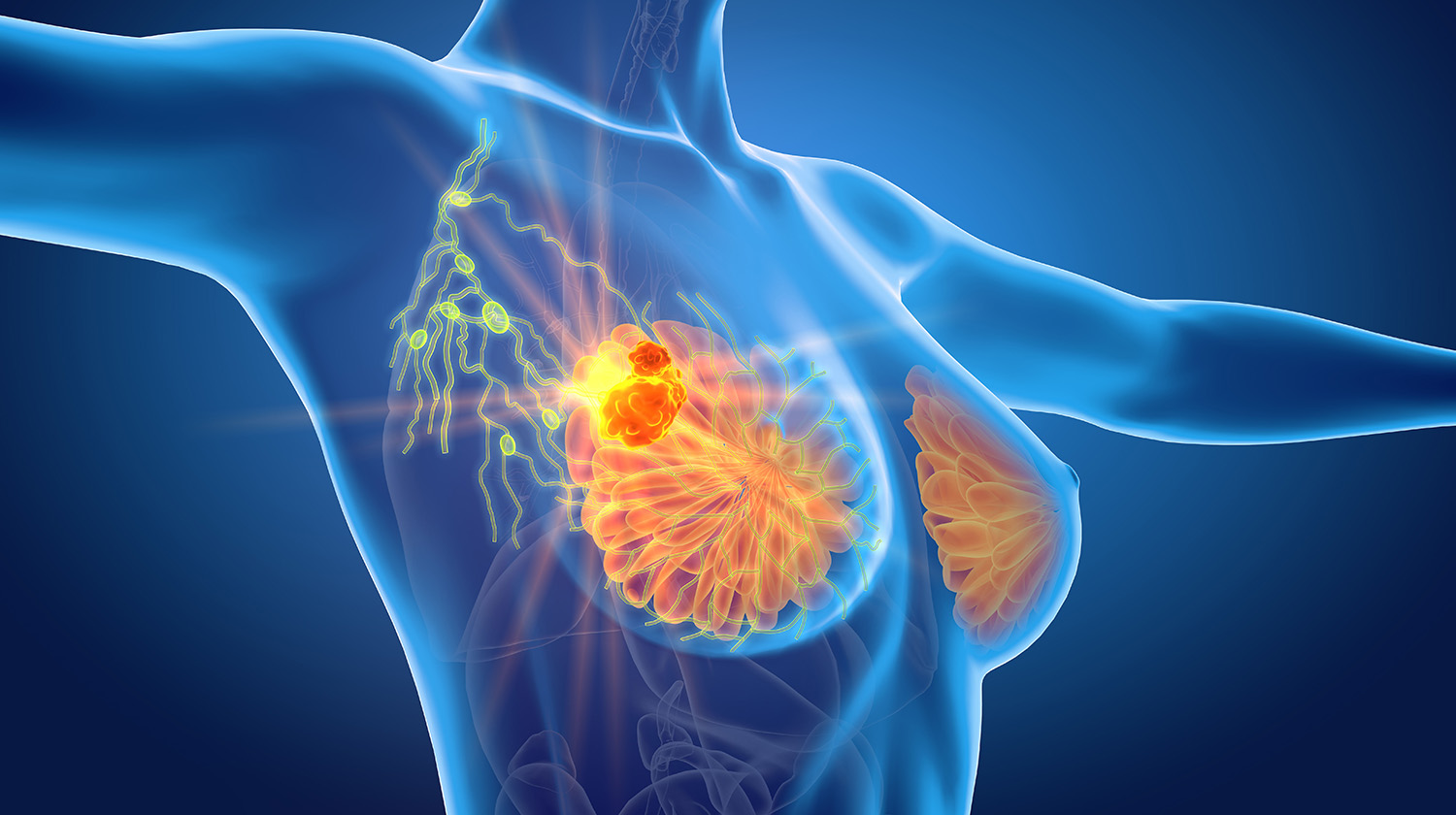
Breast Cancer
Breast cancer is the most common type of cancer affecting women globally, with 1 in 10 women developing it over their lifetimes. 81% of breast cancers occur in women over the age of 50. Exactly why some women get breast cancer while others don’t remain unknown. However, research suggests that breast cancer is caused by a combination of factors, some of which are beyond control.
Most breast cancers happen by chance. Despite this, approximately 5% of people diagnosed with breast cancer have an inherited genetic fault. Of the known breast cancer genes BRCA1, BRCA2, or TP53 are the most common. The three main risk factors for breast cancer are gender (being female), age (risk increases after age of 50), and significant family history (particularly when first-degree relatives are involved i.e., parent or sibling).
Other observed risk factors for breast cancer that have less significance, include a previous personal history of breast cancer, increased hormonal exposure such as early menarche (first period) or late menopause, and lifestyle (obesity, excessive alcohol intake, smoking, and diabetes).